Mental health claims face growing scrutiny
Reprints
Employers and insurers are more likely to challenge the treatment of mental injury claims as workers compensation systems see an increase in claims with a psychological element, experts say.
Although fewer mental injury claims are denied outright as states expand comp presumptions for workplace psychological injuries, treatment for those claims is more heavily scrutinized through dispute mechanisms such as independent medical evaluations.
In addition, special expertise is needed to evaluate mental injuries, which complicates the claims and evaluation process.
“There’s always been some skepticism around mental health claims in the work comp environment,” said Michele Tucker, a San Francisco-based vice president with Marsh LLC.
Hard data on mental reviews is hard to find, but a report from the California Division of Workers’ Compensation shows that treatment requests in the state that are most often overturned during the independent medical review process are for behavioral and mental health services out of all treatment service categories.
California figures show that while mental and behavioral health service requests increased between 2020 and 2022, overall independent medical review activity decreased during that same time frame.
Mental health independent medical reviews can be a paperwork task – collecting information from claimants’ medical records – which occurs when there is a challenge to recommended treatment, said Chattanooga, Tennessee-based Les Kertay, behavioral health medical director for Genex Services, an Enlyte LLC company.
But in-person exams can also be scheduled if injury causation is queried, Mr. Kertay said. In those cases, clinicians conducting independent medical reviews vary by state, with jurisdictions either requiring the professionals conducting the reviews to be psychiatrists or clinical psychologists, he said.
“In mental health, we typically have symptoms and observations, but there really aren’t hard signs,” he said. “There’s not a blood test. I think that complicates things and makes it more likely that people will have some degree of skepticism.”
But outright denying claims can be difficult, and the comp industry is denying or disputing fewer mental health claims than in the past, Ms. Tucker said.
One reason fewer mental health claims are being denied is the expansion of mental injury comp presumptions, said Alex Swedlow, president of the California Workers’ Compensation Institute. Numerous states have expanded presumptions to include conditions such as post-traumatic stress disorder (see related story below).
“There would be a logical conclusion that as the number of mental health cases goes up, from conclusive presumptions, so will psychiatric services,” Mr. Swedlow said.
Most of the presumptions apply to first responders, but Connecticut created a mental injury presumption for all employees.
While there remains skepticism about the claims, some comp experts say the increase in mental injury comp claim acceptance reflects societal shifts regarding psychological health.
“We have a mental health crisis in this country. Is that going to weave its way into workers comp? Absolutely,” said David Langham, Florida’s deputy chief judge of workers compensation claims.
Proving mental injuries resulted from the workplace can be difficult, and those questions are “inherently going to lead into the independent medical examination process,” Judge Langham said.
The use of procedures such as utilization reviews and independent medical evaluations in claims involving mental injuries is likely to increase, Ms. Tucker said.
Independent medical reviews typically come after utilization reviews and peer reviews have been exhausted, and are traditionally rarer in treatment disputes, said Atlanta-based Alex O’Neal, CEO of Arbicare LLC, a utilization management services company.
When treatment challenges involve behavioral and mental health claims, it can be difficult for claims professionals, who are often not clinically trained, to understand whether mental injuries relate to underlying psychological issues or stem from workplace injuries, he said.
“Did whatever happened that caused that injury help create these mental health issues and these mental health disorders or were they preexisting and already a part of that person’s normal, ongoing life,” Mr. O’Neal said. “That is a really challenging thing to understand.”
When addressing mental injury treatment appropriateness, confusion can stem from whether a condition is strictly physical, strictly mental, or both, said Kenji Saito, Augusta, Maine-based president of the American College of Occupational and Environmental Medicine.
Some physical conditions can also lead to secondary mental health issues, he said, adding that the most common reason behind treatment denial in mental health claims is improper diagnosis.
“The challenge is, we don’t have good long-term outcome studies on a lot of these treatment modalities,” he said. “There are going to be a lot of what-ifs until we really define what do we mean in terms of diagnosis.”
Comp presumptions expand, pushing boundaries of mental injury benefits
As mental injury workers compensation claims rise, some experts point to expanding psychological injury presumptions in many states as a reason.
Several states have added conditions such as post-traumatic stress disorder as presumptive occupational injuries, a movement that some attribute to legislators’ reaction to work-related issues experienced by first responders and others during the COVID-19 pandemic.
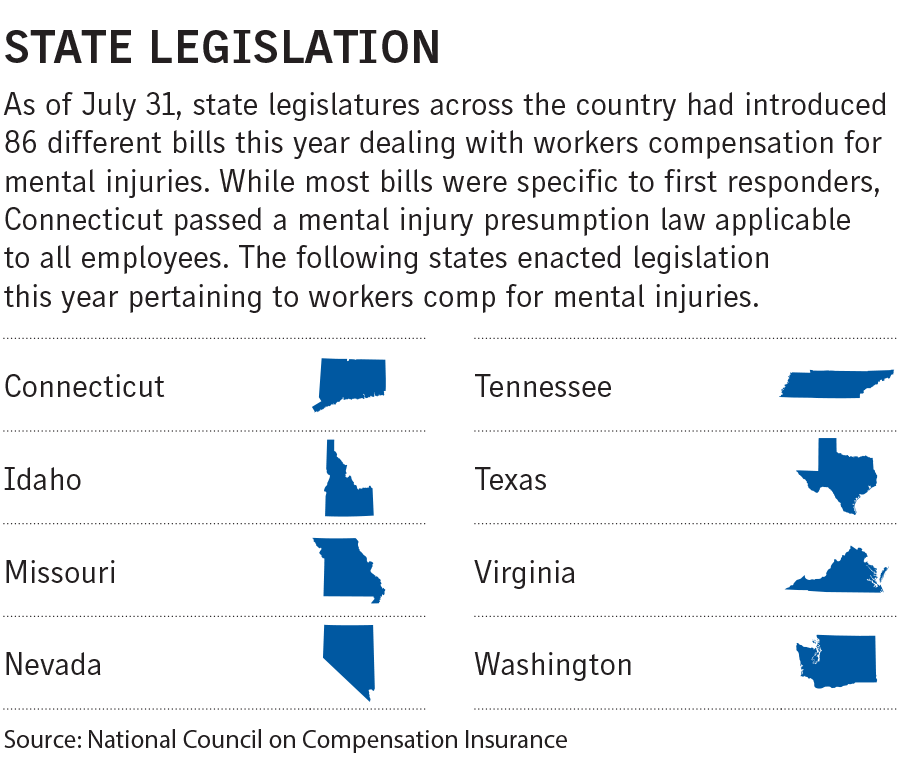
This year, eight states created presumptions or enhanced existing ones, following the 25 states that have laws that simplify the process for mental injuries in workers comp. Most of the laws require that a worker witness a qualifying traumatic incident, such as a death, to qualify for benefits, and some can be rebutted if it is proven that the mental injury was not caused by work.
“Some people feel (presumptions are) really growing in intensity,” said Alex Swedlow, president of the California Workers’ Compensation Institute.
Presumption laws for mental injuries are expanding due to greater societal focus on psychological health and the loosening of the stigmas surrounding the issue, said Chattanooga, Tennessee-based Les Kertay, behavioral health medical director for Genex Services, an Enlyte LLC company.
While many states have expanded mental injury presumptions for first responders, Connecticut this year went a step further and introduced a presumption for all employees, a move experts say could lead to the filing of more mental health claims and possibly more cases of independent medical review when treatment is challenged.