First impressions matter in comp claims
Reprints
Workers compensation experts say that trust in the workplace and early positive communication between injured workers and their employers or claims handlers can play a crucial role in reducing the time it takes a claimant to return to work, as well as keeping comp claim costs in check.
“Showing that you care about your employee’s wellbeing, letting the individual know you are sorry that the injury happened, checking in frequently, and showing that you are there for them throughout the process will go a long way towards establishing trust,” said Erica Fichter, Miami-based senior vice president, medical management with third-party administrator Broadspire Services Inc.
Lack of trust in the workplace means that an injured worker may fear being fired or laid off — employees with these fears tend to have worse outcomes, according to research from the Workers Compensation Research Institute.
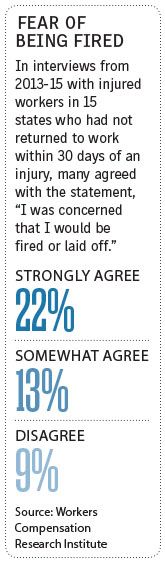
Cambridge, Massachusetts-based WCRI said in a 2010 report that 22% of workers who feared for their job security had no substantial return to work for at least 30 days post-injury.
Workers who fear being fired or laid off also were more likely to hire attorneys, the study found.
Joseph Paduda, Skaneateles, New York-based principal at Health Strategy Associates L.L.C., says there has been a fundamental change in the relationship between workers and employers in the past 20 years that has fueled workers’ fears of losing their jobs.
“In many corporations, workers are no longer seen as a valuable asset, as a key to the success of the organization. They are seen as costs,” he said.
Experts say that positive contact between an injured worker and their supervisors and claims handlers in the immediate aftermath of a work injury can determine the outcome of a workers comp claim by allaying some of those job fears.
“Creating an environment of goodwill and caring can lessen the client’s loss costs, improve medical treatment compliance, decrease disability durations, increase closures and decrease litigation,” Ms. Fichter said.
Claims handlers whose first contacts are positive or seemed supportive had better outcomes, according to a study released in 2012 by the Liberty Mutual Research Institute for Safety in Hopkinton, Massachusetts. Average claim costs went down to $3,913 from $6,619 for claims that involved positive interactions, while the average duration of the claim went down from 33.5 days to 14.1 days, the report found. Medical costs also went down to $2,344 from $3,378 when claims handlers focused on positive initial communication, Liberty Mutual said.
“How their workplace supervisor responded to them when they first came and said ‘I’m hurt’ had a very significant impact on outcomes. The key negative responses that drove outcomes were: being not supportive, blaming them for their injury, being angry at them, not believing that they were injured or telling them not to file a workers comp claim,” said Dr. Glenn Pransky, director of the Center for Disability Research at the Liberty Mutual safety institute. Dr. Pransky presented the findings during a presentation last month at WCRI’s Annual Issues & Research Conference in Boston.
Dr. Pransky added that employers that showed more than one negative response saw injured workers stay out of work twice as long as people who didn’t receive a negative response.
“A lot of this comes down to how people perceive they’re being treated and how they perceive they are being valued by the organizations,” Mr. Paduda said.
Mr. Paduda said companies such as Issaquah, Washington-based Costco Wholesale Corp. and Mooresville, North Carolina-based home improvement retailer Lowe’s Cos. Inc. have created more positive early interactions by assigning nurses to talk with injured workers about their medical issues, return to work and any other questions.
Meanwhile, claims adjusters focus on other claim-related issues such as investigation, reporting, reserving and legal aspects of the claim. Nurses and claims adjusters share information and collaborate to ensure all parties are working toward the same objectives.
“When you think about it, nurses are trained to care for people. They are trained to ask questions, be supportive, to respect where people are coming from,” Mr. Paduda said.
Mr. Paduda said nurses would approach communication differently than a claims handler “who first wants to make sure that the claim is appropriate, so they are going to ask questions about: where did the injury occur, who saw it, what were you doing when the injury occurred? A patient who just got hurt may well feel that they are being questioned about whether they got hurt at work, whether they are lying.” A culture of positive interactions should begin even before a work accident has occurred, said Stephen Peacock, St. Louis, Missouri-based assistant vice president of claims with excess workers compensation insurer Safety National Casualty Corp.
“They know they need to establish a good relationship with their employees, so they feel comfortable and respected enough to not be afraid to report accidents at work,” he said.
Maintaining social interaction “is a very important point that most employers overlook,” said Rob Schiller, Philadelphiabased assistant vice president of claims with AmTrust North America, during the Philly I-Day 2017 conference last month.
Injured employees “miss the camaraderie” with their co-workers when they are out of work, he said.
“A lot of employees feel like they’re not part of the employer anymore,” Mr. Schiller said. “You want to maintain that interaction. You want the supervisor to continue to reach out to the injured workers to see how they’re doing.” Isolation also is a challenge for injured workers, said Jane Lamb, Philadelphiabased director of risk management for Philadelphia Gas Works, during the Philly I-Day conference.
“It’s hard to come back,” she said.
Gloria Gonzalez contributed to this report.
Read Next
-
Empathy, measured approach can aid claims communication
Claims handlers can take several steps to have positive communication with workers compensation claimants, ultimately improving claim outcomes, said Dr. Glenn Pransky, director of the Center for Disability Research at the Liberty Mutual Research Institute for Safety in Hopkinton, Massachusetts.