Battle over health insurance premium subsidies may dilute Affordable Care Act
Crucial ACA provision faces legal hurdles Reprints
The ultimate outcome of lawsuits seeking to limit the availability of federal premium subsidies under the health care reform law could substantially weaken its key provisions, including the employer and individual coverage mandates.
In rulings late last month, panels of the U.S. Court of Appeals for the District of Columbia and the 4th U.S. Circuit Court of Appeals in Richmond, Virginia, issued opposite decisions on whether the Patient Protection and Affordable Care Act expressly limits subsidies to health coverage bought through state-operated public insurance exchanges.
In its July 22 ruling in Jacqueline Halbig et al. v. Sylvia Mathews Burwell et al., the D.C. Circuit panel ruled 2-1 that it does.
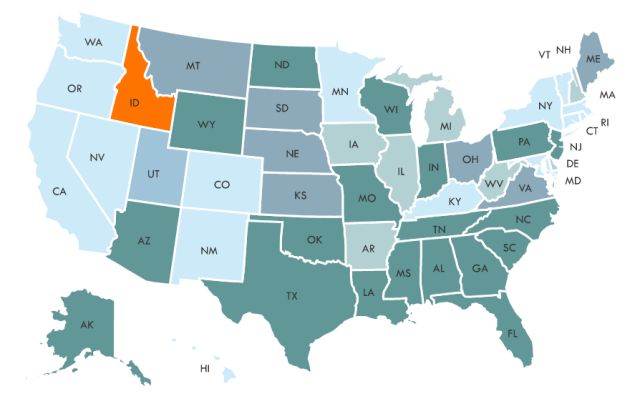
That same day, the 4th Circuit panel concluded unanimously in David King et al. v. Sylvia Mathews Burwell et al. that the reform law wording is ambiguous enough to allow premium subsidies for coverage bought through state and federal public health insurance exchanges. The federal exchange covers 36 states that did not establish their own exchanges.
Experts say the opposing rulings add new layers of uncertainty for enforcing ACA coverage requirements for employers, which are due to take effect next year, as well as the long-term viability of the public exchanges (see related story).
“The implications of this are pretty profound,” said Frank Fanshawe, an Albany, New York-based partner at Wilson Elser Moskowitz Edelman & Dicker L.L.P.
Under the ACA, employers that fail to provide affordable health care coverage to 70% of their full-time workforce in 2015 and 95% of full-time workers in 2016 would be penalized only if an employee buys subsidized coverage through a public exchange.
“In the absence of those subsidies in the federal exchange, the employer coverage mandate would effectively disappear in the states that aren't running their own exchange,” Mr. Fanshawe said.
However, experts say only employers with full-time workforce populations living solely in states that rely on the federal exchange would be insulated from the coverage penalty if the District of Columbia circuit's ruling is ultimately upheld. An employer still could be penalized if an employee lives in a state that runs its own exchange and uses the federal subsidy to buy coverage.
“That would wind up triggering the employer mandate penalty if you're not offering coverage to a sufficient number of your employees,” said Paul Hamburger, partner and co-chair of the employee benefits, executive compensation and ERISA litigation practice center at Proskauer Rose L.L.P. in Washington. “And that penalty would be multiplied by all of your employees, not just the ones living in that state.”
In 2015, the penalty for not offering affordable coverage is to be $2,000 for each full-time employee, minus the first 80 employees; in 2016 and later, the first 30 employees are to be excluded in calculating the penalty.
Experts also say if a final ruling, presumably by the U.S. Supreme Court, shields employers with workforces confined entirely to states without an exchange, that protection may be short-lived.
If the subsidies are eventually limited to consumers using the state-based exchanges, “the big question is what happens with the states that aren't currently running their own exchanges,” said H. Guy Collier, a Washington-based partner at McDermott Will & Emery L.L.P. “One possibility is that some of those states will look at this and recognize that they have tens of thousands of citizens who really can't afford coverage without the subsidies and, despite their philosophical objections to the health care reform law, elect to set up a state-based exchange.”
Most experts agree the final word on the premium subsidies will rest with the U.S. Supreme Court, as Congress is unlikely to agree on revising the law.
How long it will take to resolve the issue in the courts is unclear. The Obama administration said it would seek a rehearing before the entire District of Columbia court in Halbig. The plaintiffs in King appealed to the Supreme Court last week.
“We're probably at least a year away from getting any sort of finality,” said Sarah Bassler Millar, partner and vice chair of the employee benefits and executive compensation practice group at Drinker Biddle & Reath L.L.P. in Chicago.
Until then, the government said it will continue providing premium subsidies through the federal exchange. Experts say employers would be well-advised to continue preparing their health benefit programs to comply with the reform law's coverage requirements.
“Employers need to assume that the law will still apply and, unless they have a strong enough aversion to this law that they're willing to test it themselves, I suspect that most employers are going to continue to do just that,” said Jay Kirschbaum, St. Louis-based practice leader of Willis North America Inc.'s human capital practice's national legal and research group.
“That's going to be the best course of action, whichever way this pans out,” he said. “If the mandate goes away, then it goes away. You'll only have incurred some additional benefits costs and administrative expenses. But if it stays in place, then you're looking at some pretty serious penalties.”
Read Next
-
Health reform law may unravel if D.C. Circuit ruling on premium subsidies stands
Individual plaintiffs in Jacqueline Halbig et al. v. Sylvia Mathews Burwell et al. and David King et al. v. Sylvia Mathews Burwell et al. — all of whom live in states that do not run their own public health insurance exchanges — allege that the IRS unfairly subjected them to the reform law's minimum essential coverage requirement by making the premium subsidies available through the federal exchange.